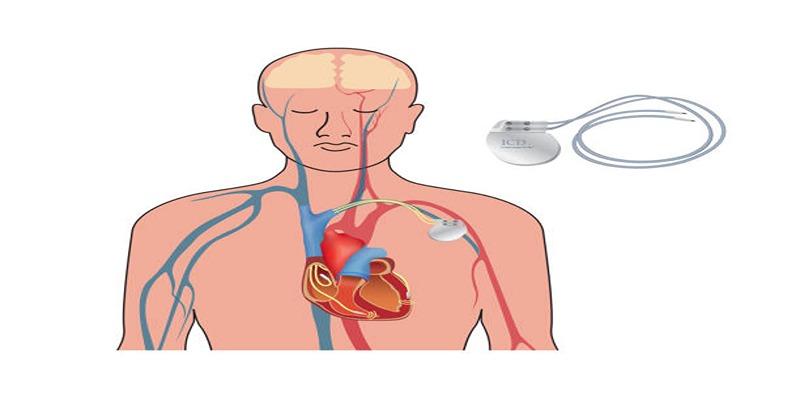
Undergoing an Implantable Cardioverter Defibrillator (ICD) procedure can feel overwhelming, especially if this is your first experience with a cardiac device. This guide outlines what typically happens before the procedure, from early evaluations to practical preparation steps, so you know what lies ahead and can approach the process with more confidence.
Initial Medical Evaluation
Your preparation usually begins with a detailed medical evaluation. Rather than being a single checklist, this stage helps your care team understand your overall health and tailor the ICD implantation to your specific situation.
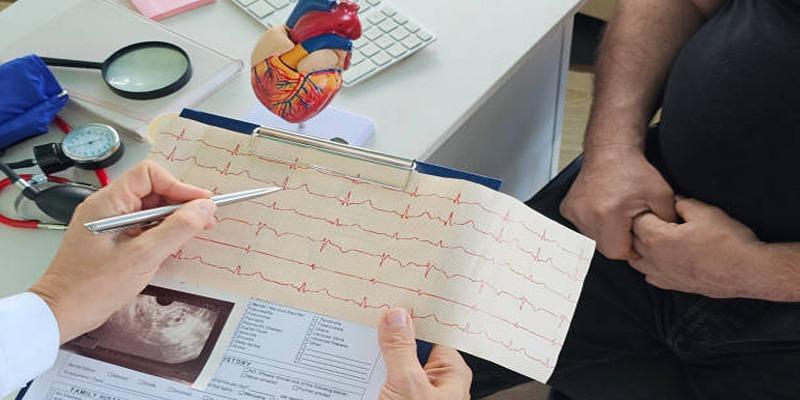
Review of Medical History
Your healthcare team will review your medical history, including any chronic conditions, previous surgeries, and family history of heart disease. These details help identify factors that could influence the procedure or recovery. Providing accurate and complete information allows your team to plan more effectively and reduce unexpected risks.
Physical Examination
A physical examination helps assess your general health. Your doctor will typically check your blood pressure, heart sounds, lung function, and circulation. These findings support decisions about anesthesia, device placement, and overall procedural planning.
Discussion of Symptoms
You will also be asked about recent symptoms such as fainting, chest pain, or irregular heartbeats. Even symptoms that seem minor can provide important context. Sharing clear timelines and descriptions helps your provider anticipate potential concerns during the procedure.
Your doctor will review all medications you take, including prescriptions, over-the-counter medicines, and supplements. This step is important for avoiding interactions with anesthesia or procedural medications. In some cases, adjustments may be recommended ahead of time to improve safety.
Diagnostic Tests You May Undergo
In addition to the clinical evaluation, diagnostic testing provides objective information about your heart and overall health. Not every patient needs every test, but several are commonly used before an ICD implant.
Electrocardiogram (ECG)
An electrocardiogram records the electrical activity of your heart. It can identify abnormal rhythms, prior heart damage, or conduction issues that may influence procedural planning. The test is quick, non-invasive, and routinely performed.
Echocardiogram
An echocardiogram uses ultrasound to create images of the heart. It allows your care team to assess heart structure, valve function, and pumping strength. This information is especially helpful when evaluating heart muscle weakness or structural abnormalities.
Holter Monitor
A Holter monitor records heart rhythms over an extended period, often 24 hours or longer. This can reveal irregular rhythms that may not appear during a brief ECG. Your doctor may suggest this test if symptoms occur intermittently.
Stress Test
A stress test evaluates how your heart responds to physical activity. It can show whether the heart receives enough blood under stress and helps your care team understand how your heart performs in everyday conditions.
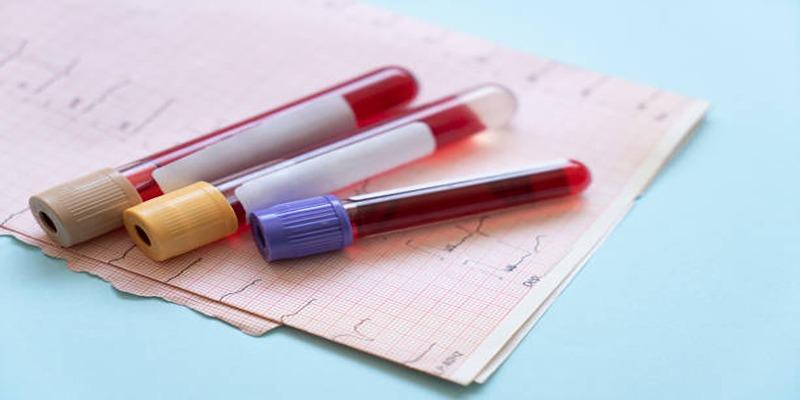
Blood Tests
Blood tests are used to evaluate kidney function, electrolyte balance, and clotting ability. These results help determine how well your body can tolerate medications and recover after the procedure. Abnormal findings may lead to temporary adjustments in your care plan.
Advanced Imaging
In some cases, advanced imaging such as CT scans or MRI may be recommended. These tests provide more detailed views of heart structures or surrounding anatomy and can be useful when additional clarity is needed.
Pre-Procedure Instructions
Before the procedure, your care team will provide specific instructions. Following them closely helps reduce complications and ensures your body is ready.
You are usually asked not to eat or drink for six to eight hours before the procedure. This reduces the risk of complications during anesthesia and is a standard safety precaution.
Some medications, including blood thinners or diabetes treatments, may need to be paused or adjusted. These changes are made to reduce bleeding risk or prevent blood sugar issues while fasting. Always follow the guidance provided by your healthcare team rather than making changes on your own.
On the day of the procedure, bring identification, insurance information, and an up-to-date list of medications with dosages. If requested, include relevant medical records. Small comfort items, such as a phone charger, may also be helpful during recovery.
Understanding Anesthesia and Sedation
Most ICD procedures use local anesthesia combined with sedation. The anesthetic numbs the area where the device is implanted, while sedation helps you stay relaxed. Depending on the level used, you may feel drowsy or lightly asleep, and many patients remember little of the procedure.
It is important to tell your provider about any allergies or previous reactions to anesthesia. This information allows the anesthesia team to select the safest approach for you.
Preparing Mentally and Emotionally
Mental preparation is often overlooked but can make the experience easier. Simple relaxation techniques, such as deep breathing or guided imagery, may help reduce anxiety. Discussing concerns with your care team can also provide reassurance and clarity.
Support from family or friends can be helpful during this time. Feeling emotionally supported often makes the overall process feel more manageable.
Physical Preparation for the Procedure
Physical readiness supports recovery. Following instructions about fasting, medication use, and rest allows your body to respond better to the procedure. Adequate sleep in the days leading up to surgery can also aid healing.
Conclusion
Preparing for an ICD implant becomes more manageable when you understand each step in advance. Medical evaluations, diagnostic testing, and careful preparation all play a role in improving safety and outcomes. By following instructions and addressing both physical and emotional readiness, you can approach the procedure with greater confidence and clarity.